When it comes to understanding brain health, many might not immediately think of hormones, particularly those originating from the gut. Yet, the intricate interplay between our gastrointestinal system and our brain — often referred to as the gut-brain axis — plays a pivotal role in regulating numerous cognitive functions and overall neural health. Central to this relationship is the incretin effect, mediated by two key hormones: GIP and GLP-1. These hormones not only help manage our blood sugar levels but also exert significant influence on our brain’s health and function.
Contents
Understanding Hormones: GIP and GLP-1
The intricate web of hormones within our bodies is vast, with each hormone playing a unique role in maintaining physiological balance. Among these myriad hormones, incretins, specifically GIP and GLP-1, are noteworthy not just for their primary functions, but for their wider implications in the realm of neural health.
What are Incretins?
Incretins are a group of metabolic hormones that play a crucial role in the regulation of glucose metabolism, primarily by amplifying the secretion of insulin post-meal. These hormones are released from the intestines and offer a snapshot into the dynamic relationship between our gut and other bodily systems.
Definition and Role in the Body
Gastric inhibitory polypeptide (GIP) and glucagon-like peptide-1 (GLP-1) are the primary incretins found in humans. They are both peptides, meaning they are constructed from amino acids, and are secreted in response to nutrient ingestion. Once released, they play a vital role in maintaining glucose homeostasis by promoting insulin secretion, thus ensuring that the sugar from our meals is used efficiently by our cells.
Main Types: GIP and GLP-1
While GIP and GLP-1 share many similarities, they also have unique characteristics. GIP is primarily secreted by K cells located in the upper part of the small intestine, specifically the duodenum and jejunum. In contrast, L cells, found throughout the intestines but concentrated in the ileum and colon, secrete GLP-1. Although they arise from different regions of the gut, they converge in their function to modulate glucose metabolism, amongst other roles [1].
Production and Secretion of GIP and GLP-1
To better appreciate the importance of these incretins, it’s essential to understand the conditions under which they’re released and how they’re integrated into our metabolic processes.
Gastrointestinal Origins
Our gut is not just a passive tube that processes food; it is a lively ecosystem bustling with cellular activity. The specialized cells, namely the K and L cells, sense the influx of nutrients—particularly carbohydrates and fats—and respond by secreting GIP and GLP-1. This immediate response ensures that the body is prepared to handle the sudden influx of glucose post-meal.
Response to Nutrient Intake
The secretion of GIP and GLP-1 is tightly regulated and influenced by the type and amount of nutrients ingested. For example, fatty acids and certain amino acids can stimulate the release of GLP-1, whereas GIP secretion might be more responsive to oral glucose. This nuanced regulation allows for precise coordination with other metabolic hormones, ensuring our body maintains an optimal glucose balance.
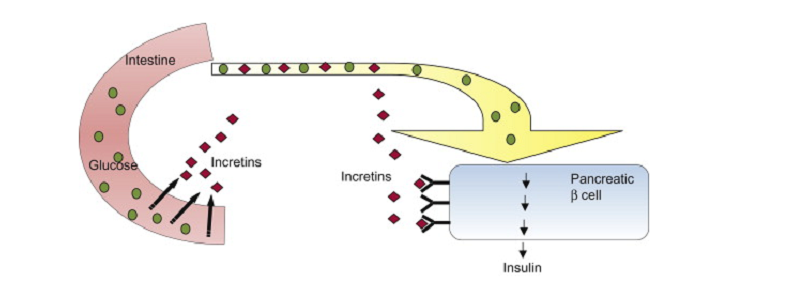
The Mechanism of the Incretin Effect
As we delve deeper into the workings of the incretin effect, it becomes apparent that the roles of GIP and GLP-1 aren’t confined to mere glucose regulation. These hormones orchestrate a symphony of metabolic responses, ensuring the body remains in balance after consuming food. The incretin effect is a cornerstone of this metabolic dance, providing insight into how these hormones contribute to both immediate and long-term physiological equilibrium.
Interaction with Insulin
Insulin, a hormone primarily produced in the pancreas, is a key player in the world of glucose metabolism. GIP and GLP-1, through the incretin effect, closely interact with insulin, ensuring that glucose from our meals is efficiently used or stored [2].
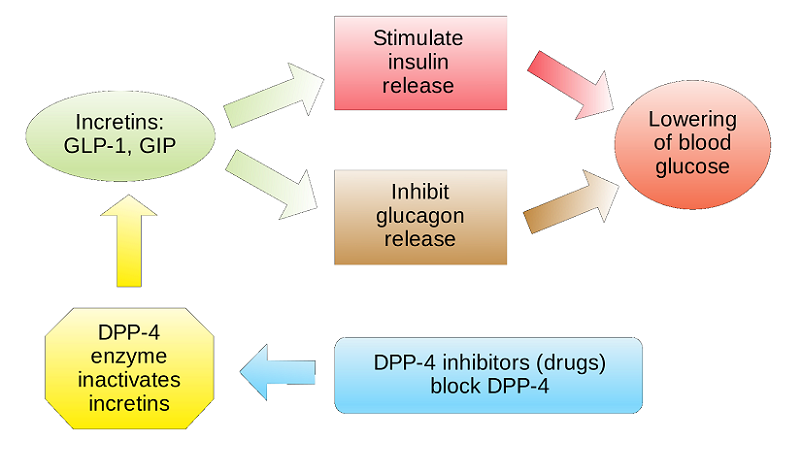
Stimulation of Insulin Secretion
Upon food intake, especially carbohydrates, blood glucose levels rise. Recognizing this spike, GIP and GLP-1 act swiftly. They bind to their respective receptors on the pancreatic β-cells, stimulating these cells to release insulin. Insulin then prompts cells throughout the body, especially in the liver and muscles, to absorb this glucose, ensuring blood sugar levels do not remain elevated for prolonged periods.
Inhibition of Glucagon Release
Equally important as promoting insulin secretion is the inhibition of glucagon—a hormone that works in opposition to insulin. While insulin promotes glucose uptake by cells, glucagon stimulates the release of glucose from storage sites, particularly the liver. Under the influence of GIP and GLP-1, glucagon’s release is curtailed, further aiding in the reduction of blood glucose levels after meals.
Effects on Blood Glucose Levels
With the delicate interplay of insulin and glucagon under the guidance of GIP and GLP-1, one might wonder about the broader implications of this orchestration on our overall glucose metabolism.
Regulation and Stability
The incretin effect ensures a smooth transition from a post-meal state of elevated blood sugar to a state of stability. By bolstering insulin secretion and inhibiting glucagon release, GIP and GLP-1 work in tandem to prevent abrupt spikes or drops in blood glucose levels. This stability is crucial, as dramatic fluctuations can be detrimental to various body systems, including the brain.
Role in Glucose Homeostasis
Homeostasis, or the maintenance of a stable internal environment, is vital for our survival. Glucose homeostasis refers to the balanced regulation of blood sugar levels, irrespective of external factors like food intake. The incretin effect, via the actions of GIP and GLP-1, is central to this balance, ensuring that our cells receive a steady supply of energy while preventing the potential harms of hyperglycemia (excessively high blood sugar) [3].
The Influence of GIP and GLP-1 on Neural Health
The brain, a marvel of biological engineering, requires a stable and nourishing environment to function optimally. While the role of GIP and GLP-1 in glucose regulation is clear, emerging research suggests that their influence extends far beyond metabolism. These hormones hold promise as agents of neuroprotection and cognitive enhancement, bridging the connection between our gut and the intricate neural networks in our brains.
Neuroprotective Effects
The concept of “neuroprotection” refers to the strategies and mechanisms that protect our brain cells, or neurons, from damage. As it turns out, GIP and GLP-1 might be unsung heroes in this arena.
Reduction of Oxidative Stress
Oxidative stress is a result of an imbalance between the production of free radicals (unstable molecules) and the body’s ability to counteract or detoxify their harmful effects. This can lead to cellular damage, especially in the sensitive environment of the brain. Both GIP and GLP-1 have been shown to possess antioxidant properties. They help neutralize free radicals and bolster the brain’s defense mechanisms against oxidative insults.
Prevention of Neuronal Death
The death of neurons can be a hallmark of various neurodegenerative diseases. Intriguingly, GIP and GLP-1 have demonstrated potential in preventing neuronal death. They achieve this through various pathways, including reducing inflammation, modulating neurotransmitter release, and even promoting the growth of new neuronal connections [4].
Cognitive Enhancements and Memory
Beyond mere protection, there’s an exciting frontier of research exploring the influence of these incretins on cognitive function and memory.
Enhancement of Learning and Memory
Studies have revealed that GLP-1, in particular, can enhance synaptic plasticity – the ability of synapses (connections between neurons) to strengthen or weaken over time. This property is fundamental for learning and memory processes. Through this and other mechanisms, both GIP and GLP-1 might play a role in improving our cognitive faculties, making them potential candidates for therapeutic interventions in conditions like Alzheimer’s disease.
Role in Neurogenesis
Neurogenesis, the process by which new neurons are formed, was once thought to be limited to early development. Recent findings, however, show that certain parts of the adult brain, especially the hippocampus (a region vital for memory), can produce new neurons. GIP and GLP-1 appear to encourage this process, further cementing their roles in cognitive health [5].
Mood and Behavior
The brain’s reach isn’t limited to cognition; it’s also the epicenter of our emotions and behavior. Here too, incretins make their mark.
Impact on Stress and Anxiety
Stress and anxiety can have profound physiological effects, and the balance of certain neurotransmitters plays a crucial role in mediating these emotions. GIP and GLP-1, through their intricate interactions with various brain regions, may help modulate stress responses and exert anxiolytic (anti-anxiety) effects.
Role in Depression and Emotional Regulation
Depression, a global health concern, is multifaceted in its origins. Emerging evidence suggests that GLP-1, in particular, may have antidepressant properties. While the mechanisms aren’t fully understood, it’s believed that incretins might influence pathways linked to mood regulation, providing a novel avenue for potential treatments.
References
[1] The effects of incretin hormones on cerebral glucose metabolism in health and disease
[2] Incretin and insulin signaling as novel therapeutic targets for Alzheimer’s and Parkinson’s disease
[3] The incretin system in healthy humans: The role of GIP and GLP-1
[4] Incretins and Amylin: Neuroendocrine Communication Between the Gut, Pancreas, and Brain
[5] Central effects of GLP-1: new opportunities for treatments of neurodegenerative diseases
